Spotting the killjoy cell
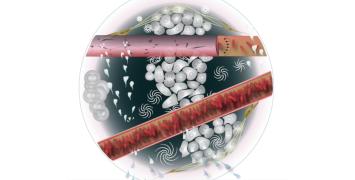
A microchip device to detect tumour cells in the blood, at a glance
There are trillions of cells in the human body of different sizes and shapes. In such a densely populated environment, the chances of detecting a single tumour cell circulating in the bloodstream, seem pretty weak. Yet, to prevent potential metastasis, responsible for 90% of cancer-related deaths, early detection is a must. Liesbet Lagae, an engineer based at Imec in Leuven, Belgium, is developing a microchip device that hunts, inspects and sorts out malignant cells circulating in the blood, sharply and cheaply.
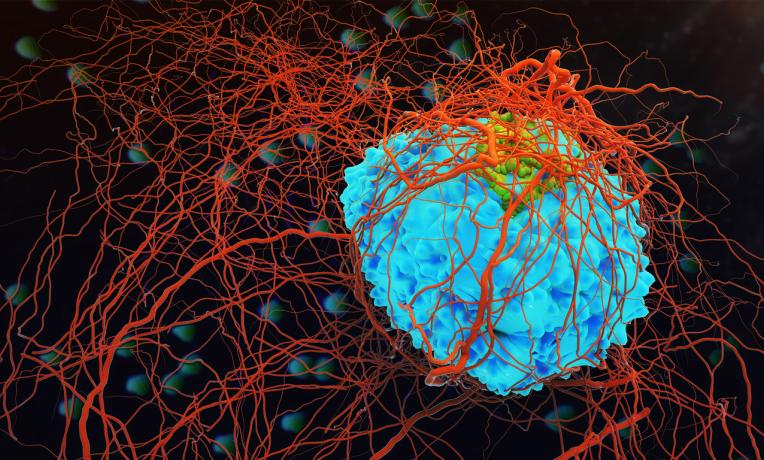
The aim is to develop a device that fits into your wallet and is cheaper, safe and faster than any existing cell sorter technology. Equipped with a 2D digital imaging system and a microfluid made of microscopic bubbles, the device will be able to analyse up to 20 million cells per minute.
“Today, cancer patients have to go through a biopsy, i.e. cutting into the body tissue. It is the only way to identify the characteristics of the cancer and to develop targeted treatment. With this device, a simple blood test will be sufficient. The nano-electronic chip will spot very rare cancer cells circulating into the bloodstream, separate them from the healthy ones and give us all the information we need on the tumour specificities, including where it started in the body and how it mutates”, explains Liesbet Lagae.
Watching this video you are accepting Youtube cookies policy
Pictures and bubbles
In the device, a microfluidic chip quickly analyses the physical morphology of the cells by taking 2D pictures and processing the information through complex algorithms. Once identified, the tumour cells are separated from the others thanks to a thermal vapor bubble jet flow technique that takes inspiration from ink jet printers:
“Like a ink jet printer that spreads ink bubbles on a paper, we create similar bubbles inside the micro device. They are the ones that, once identified at a high speed, gently push the cancer cells into specific microfluidic channels”, explains the researcher.
The device could analyse liquid biopsies for diagnostics and for facilitating the therapeutic choice, but also brings a practical solution for the latest cancer treatments, in particular the so-called personalized cell therapies. These therapies use the resources of the patient’s immune system, reprogramming the immune cells to fight the tumour. The current bottleneck relies in separating these T-cells from billions of cells in a precise, yet high throughput manner, while keeping the cells healthy. Lagae’s cell sorter device could provide essential information on these immune cells, and because of the parallelization power offered by nanoelectronic chip technology, rapidly sort billions of patient cells to find those precious immune cells that can be used for the treatment.
<
Watching this video you are accepting Youtube cookies policy
From basic research to the market
It took four years to Liesbet Lagae and her team to develop the technique behind the cell-sorter device. The researchers are now working with clinical partners in KULeuven as well as with several companies working on T-Cell therapies, aiming to better identify the market needs, and to define a product roadmap to bring the cell sorter technology to the market.
“Implementing what you have dreamt of and taking it to the market to help cancer patients, is extremely rewarding. That’s what drives me every day”, says Liesbet Lagae.
Watching this video you are accepting Youtube cookies policy
Liesbet Lagae has received two grants from the European Research Council (ERC) through the EU’s framework programmes for Research & Innovation.
SCALPEL - A Single Cell AnaLysis and Sorting Platform based on Lensfree digital imaging techniques applied to Rapid Detection of Cancer, ERC-2013-CoG, Interuniversitair Micro-Electronica Centrum
JetCell - Project Microfluidic bubble JET flow CELL sorter for cell therapy, ERC-2016-PoC, Interuniversitair Micro-Electronica Centrum