Organoids in the fight against cancer
Colorectal cancer (CRC) is the second most common cause of cancer-related deaths. European researchers developed novel ex vivo three-dimensional organoid cultures that replicate genetic events in CRC, as tools to test novel therapeutics.
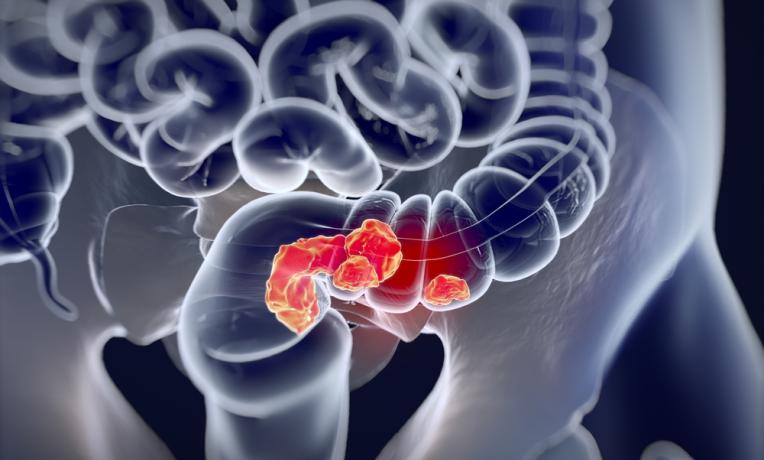
CRC emerges in the epithelium of the gastrointestinal tract, most often as a result of driver mutations in the adenomatous polyposis coli (APC) tumour suppressor gene. APC mutations increase signalling in intestinal stem cells and enhance expression of target oncogenes such as MYC (c-Myc). It is apparent that additional events are necessary for CRC development such as mutations in the KRAS and TP53 genes, which are involved in regulating key cell processes, such as the cell cycle. However, the impact of these changes on the development of CRC and response to therapy is not well understood.
To address this issue and further study CRC, ERC grantee Owen Sansom, leader of the EU-funded ColonCan project, developed a number of preclinical models that faithfully recapitulate the course of the human disease, including metastasis. “Our aim was to identify and test potential novel targets and therapies for CRC,″ explains Prof. Sansom. A key objective was to assess the impact of cooperating mutations and decipher the signalling mechanisms by which these genetic changes contribute to the phenotype of APC-deficient cells.
CRC preclinical models
Researchers utilised state of the art technologies including ribosomal and metabolic profiling to study CRC cells from their preclinical models. They discovered that KRAS mutations alter signal transduction within APC-deficient CRC cells. The project results suggested an overall increase in global protein production and alterations in nutrient stress response pathways and cellular metabolism in cells harbouring both mutations. Furthermore, they discovered that the growth factor TGF-β suppresses tumorigenesis in intestinal cells.
The scientific team also generated new mouse models of metastatic CRC using genetic engineering. Comparison of transcriptomic data generated from these models with data from human primary CRC indicated that the models recapitulate the cancer subtype with the worst overall survival. “These new models can be used to test therapeutic agents, for modelling stratified clinical trials and are an excellent platform for testing immunotherapy combinations,″ continues Prof. Sansom.
In addition, considerable effort went towards the development of organoid cultures as ex vivo CRC models or for orthotopic transplantation into mice. This new technology essentially mimics the properties and the three-dimensional structure of the tumour of origin as it emerges from tumour-initiating cells.
Novel treatments against CRC
All preclinical models were employed to test current therapies for CRC. Intriguingly, scientists observed drug resistance to many targeted therapies, suggesting that alternative approaches are urgently needed. Prof. Sansom emphasises the clinical significance of the ColonCan study “through the identification of new opportunities for treating CRC.″ Indeed targeting nutrient stress and/or metabolism has emerged as a specific approach to kill CRC cells with mutations in both APC and KRAS genes. Considering that approximately 40% of CRC patients carry both of these mutations, these findings open up new treatment avenues for late stage CRC.
Taken together, the ColonCan newly generated model systems (mice and organoids) precisely describe the human situation and will serve as powerful tools for testing new therapeutic strategies. “The ultimate aim is to use these models to drive trials of novel treatments,″ envisages Prof. Sansom. To accelerate clinical studies, researchers are working to establish a European preclinical platform for cross-validation of models and therapeutic testing in CRC.
This article was first published in CORDIS Results pack Organoids: mini organs in a dish for disease research and new cures